Increased day-to-day fluctuations in exhaled breath profiles after a rhinovirus challenge in asthma
Aim:
- To compare the day-to-day fluctuations from personal baselines in exhaled breath profiles between asthmatic and healthy controls, before and after a rhinovirus (RV) challenge.
- To investigate whether the magnitude of the altered eNose fluctuations was linked to pre-challenge inflammatory markers and was reflected in post-challenge symptoms and inflammation, to identify possible differences in biological processes between and within groups.
Take home message:The SpiroNose can detect increased fluctuations in breath profiles following a viral challenge, especially in asthma patients, even before symptoms appear. This suggests potential for early, non-invasive monitoring of asthma exacerbations, helping guide timely intervention and improving patient care.
Introduction
Asthma exacerbations, often triggered by respiratory viral infections such as rhinovirus, lead to acute episodes of respiratory symptoms and can result in emergency visits. Currently, there is a lack of predictive biomarkers for these exacerbations, especially in the pre-symptomatic phase. The analysis of volatile organic compounds (VOCs) in exhaled breath using an electronic nose (eNose) has shown potential for non-invasive monitoring of disease control. Previous studies have indicated changes in breath profiles during asthma exacerbations, but limited data exists on the day-to-day variability of these profiles, particularly after a viral trigger.
Methods
This proof-of-concept study included 12 asthmatic and 12 healthy participants, aged 18-35 years. Participants were monitored thrice weekly for 60 days before and 30 days after a standardized rhinovirus-16 (RV16) challenge. Exhaled breath was analyzed using the SpiroNose®. Day-to-day fluctuations were calculated by comparing deviations from individual baselines established during the pre-challenge period. Statistical analyses included Wilcoxon signed-rank tests, Mann-Whitney U tests, and ROC curve analysis. Correlations with inflammatory markers (e.g., IL-8, TNF-α) and clinical symptoms were assessed.
Results
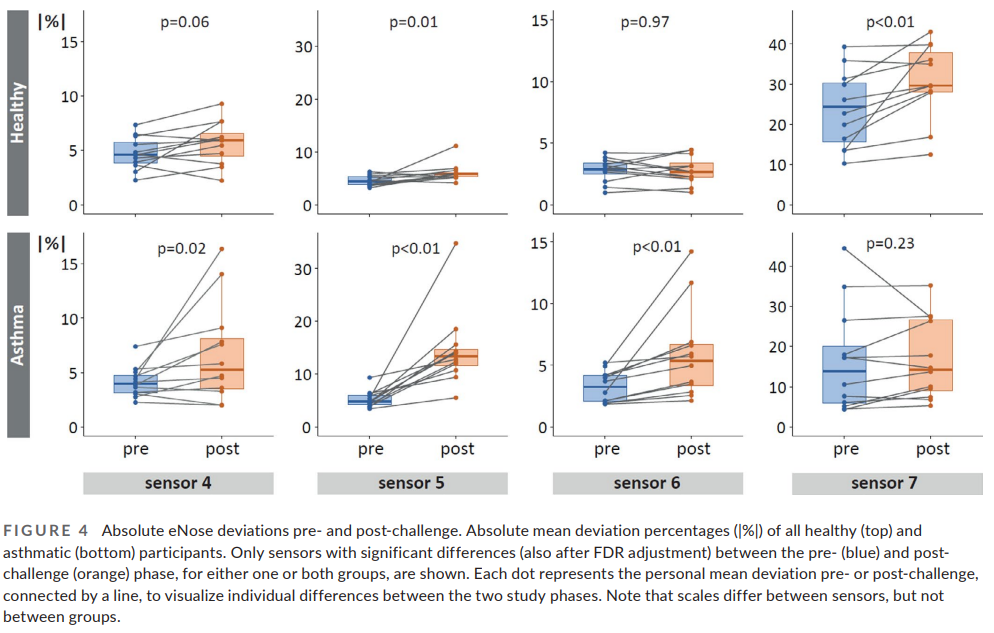
Post-challenge, both healthy and asthmatic participants showed increased fluctuations in eNose signals. In asthmatics, these fluctuations were detected as early as one day post-challenge, preceding the onset of symptoms. The eNose discriminated between pre- and post-challenge phases with high accuracy, achieving an AUROC of 0.82 in healthy and 0.97 in asthmatic participants. Fluctuations in eNose signals were moderately correlated with certain inflammatory markers (e.g., IL-8, TNF-α) in asthmatics, suggesting a link with underlying inflammatory processes.